Periodontitis is currently the most common cause of tooth loss in adults worldwide. In Germany, an estimated 80 to 90 percent of the population is affected by a mild to moderate form. The insidious aspect: the disease progresses without pain for a long time and therefore often remains undetected for years. Those who recognize the early signs and understand how periodontitis develops can take timely action and maintain healthy periodontal structures permanently.
What is periodontitis?
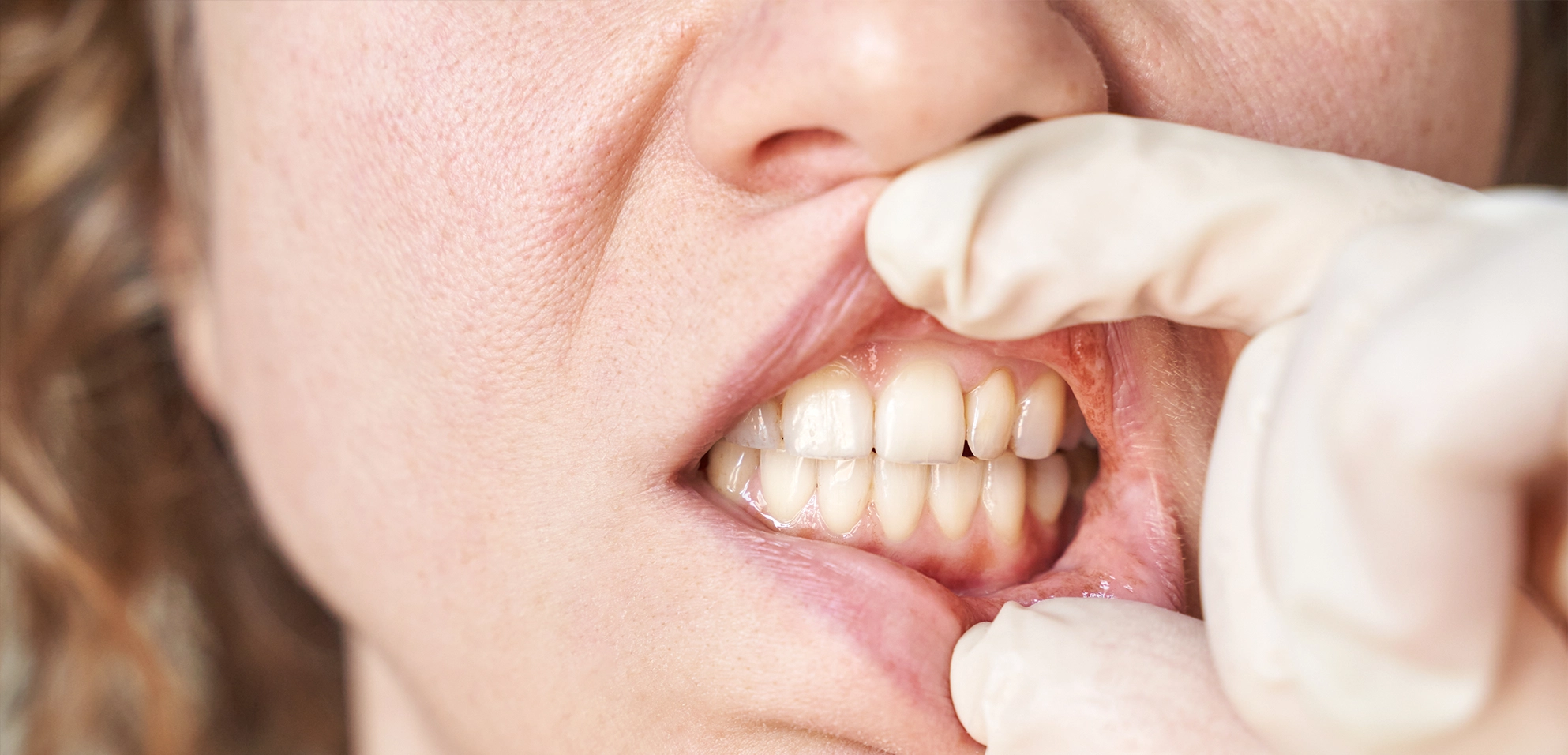
Periodontitis is a bacterial inflammation of the periodontal apparatus. The periodontal apparatus includes the gums, jawbone, root cementum, and the supporting fibers that firmly anchor the tooth in the jaw. When this supporting apparatus is destroyed by inflammation, the teeth become loose. Without treatment, they can fall out, even if they are cavity-free and externally completely intact.
Many people use the term parodontosis as a synonym. This is not entirely correct. Parodontosis describes a non-inflammatory recession of the periodontal apparatus and is hardly used medically anymore. Almost all diseases of the periodontium are inflammatory in nature and are therefore referred to as periodontitis.
How does periodontitis develop?
Sie sehen gerade einen Platzhalterinhalt von YouTube. Um auf den eigentlichen Inhalt zuzugreifen, klicken Sie auf die Schaltfläche unten. Bitte beachten Sie, dass dabei Daten an Drittanbieter weitergegeben werden.
Mehr InformationenIt all begins with dental plaque. Plaque is a thin, initially barely visible biofilm of bacteria, food particles, and saliva components that forms daily on tooth surfaces. If it is not regularly removed through thorough brushing, it hardens into tartar.
Tartar makes the tooth surface rough and provides ideal conditions for bacteria to multiply. The gums react with inflammation. They become red, swell, and bleed during brushing. This early form of the disease is called gingivitis and is still completely reversible.
If gingivitis is not treated, the bacteria migrate deeper. The gums detach from the tooth, creating so-called periodontal pockets. In these pockets, bacteria can multiply undisturbed because neither toothbrush nor dental floss can reach there. The inflammation spreads to the jawbone. The body attempts to fight off the attack and releases bone-degrading cells that ultimately destroy the periodontal apparatus itself. The teeth become loose and fall out in advanced stages.
This process progresses gradually over years. Pain often only occurs when the disease is already well advanced.
What symptoms should you be aware of?
The insidious nature of periodontitis lies in the fact that it progresses with few symptoms for a long time. Those who pay attention to the early signs can take timely action.
Typical warning signs include:
- Bleeding gums when brushing or even with light pressure
- Red, swollen, or sensitive gums
- Persistent bad breath despite good oral hygiene
- Visible gum recession and consequently longer-appearing teeth
- Sensitivity to heat, cold, or sweet foods at the tooth necks
- Loose teeth or changes in bite alignment
Bleeding gums are often dismissed as harmless. However, they are almost always a sign of inflammation and should always be taken seriously.
How is periodontitis treated?
Periodontitis cannot be cured with home remedies. It requires dental treatment that takes place in several steps.
Step 1: Diagnosis and periodontal status
We measure the depth of the periodontal pockets on each individual tooth and establish the so-called periodontal status. X-rays show how far bone loss has already progressed.
Step 2: Professional cleaning and root surface debridement
Tartar, plaque, and bacterial deposits are removed above and below the gum line. The root surfaces are smoothed so that bacteria can adhere less easily. This is the core of any periodontitis therapy.
Step 3: Monitoring and follow-up care
After treatment, we check whether the inflammation has subsided and the periodontal pockets have become shallower. In advanced cases, surgical intervention may be necessary. Regular follow-up appointments and professional teeth cleaning every three to six months ensure long-term results.
Can periodontitis be stopped? Yes. Once lost bone and periodontal apparatus cannot be completely regenerated. However, the process can be brought to a halt, and the remaining dental health can be permanently maintained.
How can periodontitis be prevented?
Periodontitis is not an inevitable disease. With consistent oral hygiene and regular professional care, the risk can be significantly reduced.
The most important daily measures:
- Brush teeth thoroughly twice daily
- Clean interdental spaces daily with dental floss or interdental brushes
- Regular professional teeth cleaning at least twice yearly
- Reduce or quit smoking
- Maintain good blood sugar control if diabetic
- Actively address stress management
Anyone who notices bleeding gums or other warning signs should not wait but schedule an appointment promptly. The earlier treatment begins, the less damage occurs.
Summary
Periodontitis develops gradually, progresses without pain for a long time, and causes considerable damage silently. Bleeding gums, bad breath, or gum recession are early warning signs that should be taken seriously.
We take this issue very seriously in our practice. Anyone who notices warning signs or wants to know the current status of their periodontal apparatus is in good hands with us. We establish the periodontal status, explain the findings clearly, and discuss the next steps together. All information about our periodontitis treatment can be found on our services page.
Frequently asked questions about periodontitis
Periodontitis is a bacterial inflammation of the periodontal apparatus. Parodontosis describes a non-inflammatory recession of the gums and is hardly used medically anymore. In everyday language, both terms are often used interchangeably, but periodontitis is almost always what is meant.
It is not completely curable. However, the disease process can be brought to a halt and the remaining dental health can be permanently maintained. The earlier treatment begins, the better the outcome.
Yes. Since 2021, systematic periodontitis treatment has been a covered service for those with statutory health insurance. The treatment is fully covered after a preliminary examination and an approved application.
This depends on the severity. Systematic treatment involves several sessions over a few weeks. This is followed by regular follow-up appointments, typically every three to six months.
The causative bacteria can be transmitted through direct saliva contact, such as through kissing or shared utensils. However, whether the disease develops depends on individual factors such as immune system, oral hygiene, and risk factors.
Bleeding gums are almost always a sign of inflammation. It does not mean that you are brushing too hard, but rather that the gums are reacting to bacteria. Anyone who regularly notices bleeding gums should schedule an appointment.
